- Locations
- Find a Physician
- By Physician
- By Department
- The Center for Spine Health
- Hand & Wrist Center
- Shoulder & Elbow Center
- Foot & Ankle Center
- Joint Replacement Center
- The Sports Medicine Center
- Pediatric Orthopedic Center
- Trauma & Fracture Center
- Osteoporosis and Bone Health
- Oncology Center
- Cartilage Repair Center
- Concussion Rehab Center
- OrthoDirect
- Careers
- Patient Portal
- Intranet
Causes of knee pain | Understanding symptoms | Diagnostics | Nonsurgical treatments | Surgical options | Joint Replacement | Knee prevention
Non-surgical Treatments
You are an active weekend warrior in your 40s and your ideal fun weekend would include two hours of tennis, some running or walking 18 holes. That is, if your arthritic knees could handle it, and they can’t anymore because your knee joint feels like bone scraping on bone. Even walking some days can be excruciating.
Worse, your orthopedic surgeon has told you that at age 40, the lifespan of an artificial knee joint, or hip joint, is about 15 years. That puts you at 55 looking at a second knee replacement surgery which gets increasingly complex, and then a third complex surgery at age 70 — all at a time when your health issues mount. The math, your doctor tells you, simply doesn’t work.
So you are stuck with knees that make climbing stairs or walking across a large parking lot appear as daunting. excruciating journey. Small comfort in that you see others your age hobbling around, as osteoarthritis affects more than 32.5 million people in the United States. According to federal data, 754,000 knee replacements and
Knee injections
Your physician may prescribe oral medications for the relief of arthritis pain or joint pain. This can include pills with Aspirin, ibuprofen and naproxen which can relieve pain and reduce inflammation.
If oral medications fail to provide relief, your orthopedic surgeon may recommend an injection of medication into the joint. An injections can offer quick, effective pain relief. However, joint injections with either cortisone, steroids or other medication have limits because over time excessive use can damage the joint.
Knee orthotics and braces
In some cases, knee pain can be alleviated by something as simple as using a foot orthotic or knee brace. Foot orthotics are orthopedic devices like insoles or supports that are usually custom fit to control the foot and correct imbalances. An orthotic foot support can raise the arch of the foot and realign the bones of the foot to prevent excess motion when you bear weight. Foot problems can sometimes cause ankle, knee, hip, and back problems.
If you are an avid runner, and you are suffering from knee problems, you may want to explore an orthotic foot device. The device could position your foot in such a way that knee pain could be alleviated.
 Many times, improper foot mechanics leads to improper running or other physical motion, and this can damage the knee. If you are suffering from arthritis, or you are overweight, the foot orthotic could help by repositioning your foot and counteracting stress on your knee to allow greater comfort and mobility for greater lengths of time. Orthotics come in rigid, semi-rigid, and soft materials. The rigid materials are generally prescribed when entire control and support is needed. The semi-rigid materials offer support, but they also allow for shock absorption.
Many times, improper foot mechanics leads to improper running or other physical motion, and this can damage the knee. If you are suffering from arthritis, or you are overweight, the foot orthotic could help by repositioning your foot and counteracting stress on your knee to allow greater comfort and mobility for greater lengths of time. Orthotics come in rigid, semi-rigid, and soft materials. The rigid materials are generally prescribed when entire control and support is needed. The semi-rigid materials offer support, but they also allow for shock absorption.
Knee braces can be used to help an existing knee injury, or to protect the knee from future injury. Before these devices are used, you should consult with a physician. If worn improperly, the brace could do damage, and wearing it for a long period of time would not allow the muscles around your knee to grow stronger.
A study from the Surgical Clinic of the Ullevaal Hospital at the University of Oslo in Norway found that patients in their study using a knee brace after anterior cruciate ligament (ACL) reconstruction had increased thigh atrophy after wearing the brace for three months.
Said another way, using a brace is like using a crutch. While it can help you become active after an injury, depending upon it excessively doesn’t encourage the supporting muscles to strengthen. And in a sense, you become dependent upon that crutch, so when it isn’t there, you can have problems.
With that said, a subliminal function of a knee brace is that it can act like a string around your finger—to remind you to be careful during activity, and not be overly aggressive with the knee joint.
Hyaluronic Acid for a degenerative knee joint
Hyaluronic acid injection is used to treat osteoarthritis. Hyaluronic acid is similar to the natural synovial fluid found in the joints. It works by acting like a lubricant and shock absorber in the joints and helps the joints to work properly.
During the procedure, the orthopedic specialist injects hyaluronic acid directly into your knee joint. The injection is repeated for up to 3 to 5 weeks. While the FDA has approved this treatment only for osteoarthritis of the knee, some use it for other arthritic joints as well as they report that it acts like lubricant in the joint.
Hyaluronic acid injections do not seem to work for all people. Those who are older or have advanced arthritis, may be less likely to find relief from these injections. Generally speaking, Hyaluronic Acid is often a last resort before more invasive knee surgery.
There can be some swelling in the knee area as a side effect of the injection. One study in 2016 in the journal Systematic Reviews found the possibility of serious side effects outweighed the benefits.
Micro-particle injection
Another non-surgical treatment option that is being explored is the use of tiny pellets that might treat arthritic knee pain, delaying the need for knee replacement surgery.
A small study by the Society of Interventional Radiology found that inserting micro-particles into small blood vessels around the knee reduced pain and improved function. The tiny micro-particles — spheres about a tenth of a millimeter in size — are made from a synthetic gel-like material. The micro-particles are inserted using a catheter run through a pinhole-sized incision, in a procedure that lasts between 45 and 90 minutes. While the research is preliminary, they have noted some patients experienced relief of symptoms from the procedure.
 Knee therapists & customized exercises
Knee therapists & customized exercises
For someone suffering knee pain the mere thought of exercise can be painful. For most knee problems specific exercises help rehabilitate injured tissues, strengthen weak muscles, and improve flexibility and range of motion.
A therapist who is specialized in knees can help an athlete rehab a partially torn ligament to avoid surgery. A knee therapist can also customize exercises that simulate the activity you hope to return to (e.g. golf, tennis, running) to strengthen the knee joint and lessen risk of injury. Same can be said for rehabilitating the knee after a surgical procedure to regain normal range of motion.
Regenerative Medicine for Knee Pain
Thankfully, for the educated healthcare consumer there is new hope with the emergence over the last 10 years of a new specialty called “regenerative medicine” that uses the body’s own healing properties to restore a knee or hip joint so that movement is less painful. The importance of this specialty is that it buys people time with their existing knee or hip joint so they are older when they consider major joint replacement surgery.
The regenerative medicine specialist harvests fat from a person’s own body, spins it down with a centrifuge and then injects the substance back into the arthritic knee joint the same day. This condensed fat providing the necessary cushion and can help the joint cartilage begin some level of healing. Within this extricated fat are important living stem cells that provide a healing function to damaged cartilage and meniscus.
The end result is that thousands of weekend athletes are back on their feet enjoying movement without pain — the same goal as surgical knee replacement but without the scalpel. The person is able to buy 10 or 20 years with regenerative medicine to reach that age where they have a good chance of outliving the lifespan of that artificial joint. The result is one joint replacement surgery rather than several risky re-do surgeries at an older age.
Buyer beware the charlatans
One of the problems, however, is that where there is a new medical advance, there is no shortage of charlatans that move in to exploit and take advantage of those who don’t do the necessary research to find the legitimate specialists in regenerative medicine.
To that end, the FDA in 2021 put out a warning that some unscrupulous clinics are bilking healthcare consumers under the tag of “regenerative medicine” when they are not providing any competence or specialization in that profession. The FDA warns that these charlatans are injecting dead stem cells harvested from other sources and charging patients exhorbitant fees for something that simply doesn’t relieve pain or provide any healing function to the joint.
With that said, the FDA also has never approved and disease-modifying drug either to provide relief from osteoarthritis, at a time when other countries have been more advanced in the use of stem cell therapy and providing helpful regenerative medicine for citizens of those countries.
There is huge demand currently in the U.S. for stem cell therapy and regenerative medicine when it is provided correctly, and FDA warning aside, that demand will continue as people try to regain movement in arthritic joints without solely depending upon a major joint replacement surgery.
There is now a growing number of respected regenerative medicine clinics and hospitals that offer stem-cell injections to relieve joint pain in a way the FDA agrees with: By extracting the body’s own bone marrow or fat, spinning it down in a centrifuge, and injecting it back the same day while the stem cells are still alive.
While the treatments are not yet covered by insurance, and the treatment can cost a few thousand dollars, thousands of these stem-cell patients have found that it works and they are back to activity without major surgery.
When insurance companies realize that the non-surgical option saves them the cost of joint replacement and all the associated rehab costs post surgery, they too will be lining up to endorse and pay for the non-surgical joint replacement option.
Consequently, the burden is on the patient to search for a reputable regenerative medicine center that can provide a non-surgical solution to their damaged knee or hip joint while they buy time to delay the need for that surgical artificial knee or hip joint replacement.
Types of Regenerative Medicine
Rather than using outside drugs, or injecting outside substances, the concept of “Regenerative Medicine” is the umbrella term for advanced methods of reversing tissue damage and REGENERATING the body by using the body’s OWN HEALING SUBSTANCES.
The term “stem cell” has varied connotations. Related to orthopedics, stem cell treatment is essentially using what cells are already in your own body, only increasing the effectiveness of your own cells.
Why a person might explore regenerative medicine and stem cell treatment over knee replacement surgery?
- It’s a minimally invasive outpatient procedure not requiring a hospital
- There are less complications and risks than surgery
- There is minimal post procedural recovery discomfort and time
- There is no use of general anesthesia
- There is no risk of rejection since the stem cells are your own, harvested from your own body.
- Stem cell treatment has proven to be effective for repairing sprained knees, tendon injuries, shoulder injuries, and other orthopedic ligament issues.
Platelet Rich Plasma (PRP) Therapy for Knee Pain
Plasma is the clear portion of the blood in which all the other blood components – platelets, red blood cells and white blood cells – travel. Each blood component has a different job.
- Red Blood Cells – responsible for carrying oxygen throughout the body
- White Blood Cells – part of the immune system that recognizes and fights bacteria and viruses
- Platelets – responsible of clotting the blood when you have an injury
Platelets have the ability to recognize damaged blood vessels. When you have a cut, platelets are drawn to the injured area where they begin to stick together to form a plug to stop the bleeding. As these platelets group together, they begin to change their shape from a disc to a spiny octopus like structure, entangling more and more platelets. These platelets, along with other proteins released within the body create a hard scab which completely stops the bleeding and protects the injury while it heals. A similar process occurs inside the body when you have a broken bone or injury that bleeds internally.
These platelets contain natural growth hormones and proteins that tell your tissues to increase rebuilding to enhance your recovery and help stop pain symptoms.
Platelet rich plasma, commonly referred to as PRP, is the patient’s own human blood that is spun down in a centrifuge and separated producing a concentration of platelets above the natural values commonly found in their blood. Platelet rich plasma can have as much as eight times more than the normal amount of platelets. This concentration of platelets from the patient’s own blood is then collected and injected back into the person at the site of injury.
The goal of PRP therapy is to enhance the body’s natural ability to repair itself to speed healing and shorten recovery time from muscle, ligament, tendon and joint injuries. PRP can be especially helpful for long-standing chronic injuries that have taken a long time to heal. Injecting concentrated platelets at the site of injury can accelerate the body’s own healing response.
PRP has been used in a variety of fields over the years, including plastic surgery, sports medicine and dermatology. Some prominent professional athletes have received PRP, including golfing great Tiger Woods and tennis champion Rafael Nadal.
There are some conflicting studies about the value of PRP, and which type of centrifuges may produce the optimal plasma. No studies to date have documented any adverse effects associated with PRP. So in that sense, there is no downside to the therapy. Because the injected platelets are produced from a person’s own body, there typically is no issue related to rejection or transmitting disease.
How is PRP administered?
A person undergoes PRP therapy in the physician’s office. The patient is instructed to stop all anti-inflammatory medication or steroids at least one week beforehand as these medications negatively affect platelets.
A small amount of blood (two tablespoons) are drawn from the patient’s arm. This blood sample is then placed into a centrifuge which spins the blood down so the heavier parts sinks to the bottom. Platelets and white blood cells spin out above this bottom layer and these concentrated platelets are collected and used for the injection.
PRP typically only requires local numbing medication at the injection site. No general anesthesia or sedation is required.
When to expect relief?
PRP does not provide instantaneous relief from symptoms. Growing new tissue and healing injured joints can take one to three months. But for those people who have seen their healing process stall, PRP can jumpstart the body’s own healing process.
There is great variability in the success of PRP based on the experience of the physician specializing in PRP, the type of centrifuge used, and selection of the ideal patient who can benefit from PRP.
Stem Cell Therapy for Knee Pain
The term “stem cell” has received a bad reputation over the years, largely due to research involving human embryos and the misperception that all stem cells come from embryos or amniotic tissues.
But, a stem cell is simply a type of cell that already exists in your body that has the unique ability to produce other cells, become a different kind of cell, or instruct other cells how to behave based on the task the body requires.
All other cells in the body are created for a specific purpose. For example, a red blood cell has the job of transporting oxygen throughout the body. But, that red blood cell is not able to divide and reproduce. Instead, when the body requires new red blood cells, it is the job of the stem cells located in your bone marrow to produce the new red blood cells. Those same stem cells can also produce white blood cells and platelets.
Stem cell therapy is the process of delivering these unspecialized stem cells to a targeted location in your body to stimulate new cell growth and tissue healing. When stem cells are injected into an arthritic joint or injured tendon or ligament, they attach to the areas of damaged tissue to initiate the healing process.
Where do stem cells come from?
Most orthopedic use cases for stem cells harvest the stem cells from the patient’s own body — from either their bone marrow or from their fat cells. While early research focused on the stem cells found in birth tissues, these types of stem cells are not typically used in an orthopedic setting.
If you are considering stem cell therapy, be sure to ask your physician what source of stem cells they plan on using.
Fat (Adipose Tissue)
Fat tissue (adipose) has become the preferred source of stem cells for multiple reasons. Adipose tissue is one of the richest sources of stem cells with 500 to 1000 times more concentration of stem cells than bone marrow. Secondly, stem cells from fat do not age and lose regenerative capability like those from bone marrow and are therefore, more effective over time. Thirdly, harvesting bone marrow through aspiration is invasive and painful. In our center, we start by using liposuction to harvest fat from the patient’s own belly region to obtain a rich source of living stem cells for more effective regenerative medicine.
Bone Marrow
Bone marrow was the first body tissue used to obtain stem cells. While harvesting bone marrow from the patient’s own body eliminates the risk of rejection and increases the likelihood the body will benefit from the injection, bone marrow stem cells are not as concentrated and are less likely to multiply and specialize compared to stem cells harvested from the patient’s own adipose tissue.
Birth Tissue (Amniotic, Placental, Umbilical Blood)
These tissues are not commonly used in orthopedic use cases.
Amniotic fluid comes from a baby’s birth sac (placenta) and can contain a small number of stem cells. But by the time that fluid is frozen and preserved for a tissue bank, and later shipped to a physician for use, there typically are no viable cells — let alone stem cells. The same is true for placental tissue and umbilical cord blood. So in reality, vials of “amniotic, placental or umbilical stem cells” are basically vials of growth factors with dead cells. And, since the cells come from a donated birth tissue and not from the patient, there is a risk of rejection. Birth tissue injections can improve pain, but, has not been shown to regrow cartilage in human studies.
How is stem cell therapy performed?
Stem cell therapy is typically performed in the office. If the physician is sourcing the stem cells from adipose (fat) tissue, the treatment will begin with liposuction to remove fat from the patient’s own belly region or buttocks. Only a small amount of tissue is harvested, so there will be no cosmetic difference to the liposuctioned area.
This collected fat tissue is processed in the office lab so the portion of the harvested tissue that contains the stem cells can be collected.
Next the physician injects the concentrated sample of stem cells into the damaged joint or tendon. The stem cells then work directly at the site of injury, or on degenerative tissue to greatly accelerate the natural healing process.
In a sense, stem cell treatment is essentially using the body’s own natural healing properties, but condensing it into a stronger dose and applying it to the body’s injured site to accelerate healing.
Stem Cell studies show promising results
While stem cells over the last 10 years stimulated a wide debate, the reality is that the therapy has become very mainstream, and is used by many professional athletes to accelerate healing so they can return to their sport.
For example, researchers at the Mayo Clinic conducted the world’s first prospective, blinded and placebo-controlled clinical study to test the benefit of using bone marrow stem cells for arthritic knee pain. It is the first time stem cells have been tested in such a rigorous fashion. The findings in The American Journal of Sports Medicine found that patients not only had a dramatic improvement in the knee that received stem cells, but also in their other knee, which also had painful arthritis but received only a saline control injection. Each of the 25 patients enrolled in the study had two bad knees, but did not know which knee received the stem cells.
A recent study showed that stem cell therapy for knee arthritis resulted in a 58-68% improvement in pain and 67-83% improvement in function one to two years after treatment. One study from 2014 showed that stem cell injections given after surgery to remove torn knee cartilage showed evidence of cartilage regeneration and lessened pain.
Are there any side effects or risks from stem cell treatment for knee pain?
Stem cell treatment for knees is noninvasive, and studies suggest that side effects are minimal. After the procedure, some people may experience temporary increased pain and swelling. However, the overwhelming majority of people who get stem cell injections have no adverse side effects.
The method where stem cells are harvested from your own body, dramatically reduces the risk of any serious side effects. However, there are various ways of harvesting and processing the stem cells, which likely affects the various success rates of the published studies.
Again, before receiving any stem cell treatment, it’s best to learn as much as you can about the physician and the stem cells they are using. There can be wide variation in success based on the physician and how experienced they are with stem cell treatment of knee pain.
Alternative Medicine
While the Alternative Medicine treatments listed here typically do not change the structure of the knee, they can relieve some pain symptoms without dependence on drugs — with virtually no side effects if done correctly. Some of these treatments may be more effective on some people than others.
Acupressure
Acupressure is an ancient Chinese form of therapy where pressure is applied to the body in order to increase blood circulation and relieve pain. This unique form of massage can relax muscles and compress nerve fibers that cause pain. If you are interested in experimenting with this form of therapy, you can either find a professional acupressure therapist or simply go to the bookstore and find a book that will tell you how to try the techniques at home by yourself or by a partner.
Acupuncture
While acupuncture has limited value for many orthopedic injuries, it may be a way of avoiding a surgery if that is your goal.
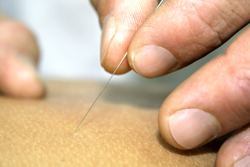 During acupuncture, hair-thin needles are inserted into various parts of the body and are stimulated to alleviate pain in many forms including but not limited to nausea, dental pain, muscle pain, menstrual cramps, and pain from osteoarthritis. This 3000-year-old Chinese art gained credibility in the western world in 1997 when the National Institutes of Health declared it to be effective for some ailments.
During acupuncture, hair-thin needles are inserted into various parts of the body and are stimulated to alleviate pain in many forms including but not limited to nausea, dental pain, muscle pain, menstrual cramps, and pain from osteoarthritis. This 3000-year-old Chinese art gained credibility in the western world in 1997 when the National Institutes of Health declared it to be effective for some ailments.
The Chinese believed that by balancing the positive and negative energy in the body, pain relief can be achieved. They found acupuncture to be an effective resource to achieve that balance. Other modern-day doctors believe that acupuncture stimulates pressure points thus releasing relaxing endorphins. Whatever the case may be, acupuncture provides relief to many people suffering from pain.
If you decide to try acupuncture, be sure to have a licensed professional administer the treatment. Also, get a physician’s referral for an acupuncturist close to you. An acupuncturist should be certified by the National Commission for the Certification of Acupuncturists. You can obtain a list of certified specialists in your area by calling the American Association of Acupuncture and Oriental Medicine.
Hydrotherapy
Spas and whirlpools are sometimes used to improve circulation and relieve chronic pain from joints. Different therapy uses different temperatures of water. Cold water reduces inflammation and warm water improves circulation.
The other aspect of working with a hydrotherapist, is that by doing exercises in a pool, the water creates an artificial weightlessness. So a very overweight person who would otherwise find any knee exercise painful because of their body weight, can find that doing exercises in a pool is tolerable.